
One of the possible treatments, the so-called adoptive cell therapy, may seem at first a slower treatment against cancer, compared to standard surgery, radiation or chemotherapy, but in principle has longer-lasting and more efficient effects to cure cancer.
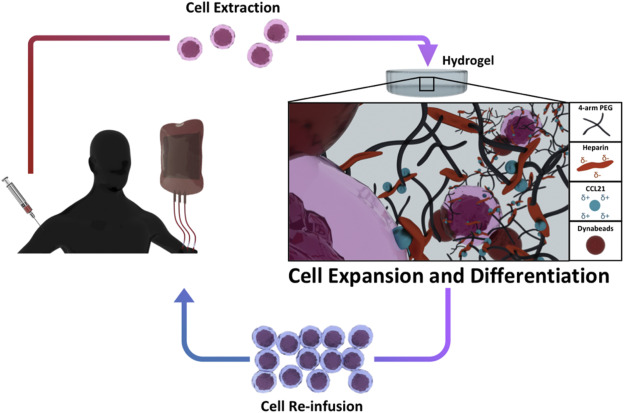
T cells (or T lymphocytes) are the cells of the immune system that have the ability to destroy cancer cells. Adoptive cell therapy involves removing these T cells from patients, modifying them to be more active, making many copies of them to have them in large numbers, and injecting them back into patients.
The application of this therapy is limited by the current cell culture media, which are not effective enough for the proliferation and growth of a relevant amount of therapeutic T cells in a short period of time and in an economically viable way, as T cells are challenging to manufacture, manipulate and control.
The 3D hydrogels designed by researchers Judith Guasch, from the Institute of Materials Science of Barcelona (ICMAB-CSIC) and Elisabeth Engel, from the Institute of Bioengineering of Catalonia (IBEC) and Professor at the Polytechnic University of Catalonia (UPC), provide higher rates of cell proliferation and capacity to select the type of cells obtained, since they are able to mimic the organs where T cells reproduce in vivo, the lymph nodes.
These 3D hydrogels are made of polyethylene glycol (PEG), a biocompatible polymer widely used in biomedicine, and heparin, a known anticoagulant agent. In this case, PEG provides the necessary structure and mechanical properties, while heparin is used to anchor the cytokine CCL21, a protein present in the lymph nodes and which has a major role in cell migration and proliferation.
This technology has recently been patented at the European Patent Office (“A synthetic hydrogel and its use for Immunotherapy and 3D-Printing”) and published in the scientific journal Biomaterials.
To continue the study and promote the transfer of this technology to the market, the two researchers have recently been awarded a project in the “CIBER-BBN 2020 Call for Transfer and Valorisation Projects”. This call is aimed at carrying out projects for CIBER-BBN groups with the interest and support of companies. The aim is to promote the transfer of scientific or technological results to the industrial sector and to provide support in marketing issues.
The project is entitled “Lymph node-inspired 3D printed hydrogels for adoptive cell therapy (Gels4ACT)”, and is led by Judith Guasch, from ICMAB, and Elisabeth Engel, from IBEC, with the collaboration of Joaquín Arribas, from the Vall d’Hebron Institute of Oncology (VHIO) and Miguel A. Mateos, from the International University of Catalonia (UIC).
The aim of the project is to print large-sized 3D hydrogels compatible with clinical bioreactors in order to expand T-cells more efficiently. The project aims to develop the laboratory prototype and carry out the first experiments for clinical phase validation.
Industrial partners are sought for further co-development, mainly biomedical and pharmaceutical companies, but also investors interested in creating a spin off to transfer this innovative technology to the market, to make it available in hospitals soon.





