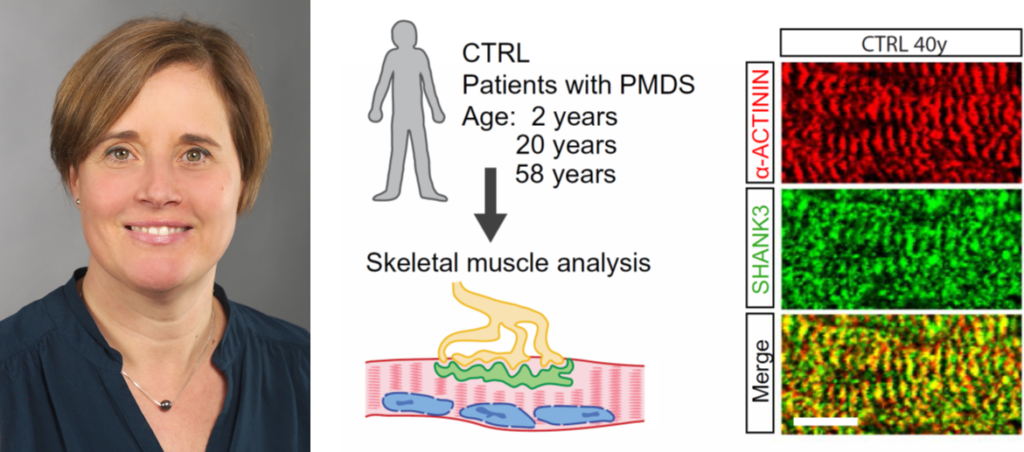
Left: Maria Demestre, expert in neuromuscular connections and associated diseases. Right: images from Maria´s last work led by Ulm University, Germany, and recently published in Sci. Transl. Med.
María, who has a degree in Biology from the Autonomous University of Barcelona (UAB), obtained her PhD in Neurophysiology from King’s College, London. Since then, she has developed an interest in neurodevelopmental and neurodegenerative disorders such as Autistic Spectrum disorders (ASD) and Amyotrophic lateral sclerosis (ALS), and in finding new tools for disease modelling and strategies for compound testing.
Maria Demestre’s expertise in these fields makes her highly valued addition to IBEC’s Smart Nano-Bio-Devices group, which develops systems, nanobots, and biosensors to treat, diagnose and monitor a variety of diseases.
I am delighted to join IBEC and to have the opportunity to contribute with my expertise to give bioengineering a biomedical approach.”
Maria Demestre
SHANK3 protein and Autism spectrum disorder (ASD)
One type of ASD in which hypotonia is commonly observed in infants is Phelan-McDermid syndrome (PMDS), which results from heterozygous deletions of the long arm of chromosome 22 (22q13.3) including SHANK3 or by a mutation on the SHANK3 gene. The resulting deficiency in SHANK3, a protein which is important in the central nervous system (CNS), leads to the social deficits seen in PMDS. In a new paper published in the prestigious journal Science Translational Medicine, it is described how deficiency of the protein SHANK3 affects the development of muscle tissues, which may lead to low muscle tone in babies and children with PMDS, that may persist till adulthood. Researchers have demonstrated that SHANK3 also plays a key role in early muscle development and maturation, suggesting that this could act as a potential therapeutic target. The study, conducted by the Institute of Anatomy and Cell Biology at Ulm University was co-led by Maria Demestre, Anne-Kathrin Lutz and Tobias Böckers.
Until now, the biological processes behind autism-associated hypotonia were not well understood. This current work describes for the first time the effect of SHANK3 deficiency on motor unit development. The study found that our bodies require SHANK3 protein not just to carry out processes in the CNS, but also to help our muscles grow and mature. In fact, a lack of SHANK3 disrupts all elements of the voluntary motor system, including motor neurons, neuromuscular junctions and striated muscles. With this discovery, the researchers have uncovered what may cause of low muscle tone in patients with PMDS.
More specifically, SHANK3 deficiency caused several important defects in the motor unit, such as shortened Z-discs (a basic unit of muscle tissue), and reduced clustering of acetylcholine receptor (which is involved in muscle contraction) in patient-derived stem cells. The researchers confirmed that this was linked to the low muscle tone seen in patients by analysing mice with alterations on the SHANK3 gene, and muscle biopsies from PMDS patients of different ages. In the latter, reduced SHANK3 was observed in an infant with PMDS compared with controls, but not in adult patients, possibly due to natural compensatory processes.
A new therapeutic target
These motor unit defects could feed back to the CNS and have an influence on the patient’s social development. In addition to this, previous studies have shown that motor deficits can impair the development of social interaction in children with ASDs. Therefore, the authors suggest that therapeutic strategies targeting hypotonia could be highly promising in the treatment of infants and children with PMDS. They found that administering either lithium or Tirasemtiv, a drug that activates skeletal muscles, improved muscle tone in SHANK3-deficient mice. Further clinical research will be needed to explore this potential therapeutic avenue and its effects on the physiological, cognitive and social development of people with PMDS.
This research offers a possible biological explanation for the hypotonia observed in infants with Phelan-McDermid syndrome—that is, that SHANK3 protein deficiency disrupts motor unit maturation.
Maria Demestre
Reference article:
A.-K. Lutz, S. Pfaender, B. Incearap, V. Ioannidis, I. Ottonelli, K. J. Föhr, J. Cammerer, M. Zoller, J. Higelin, F. Giona, M. Stetter, N. Stoecker, N. O. Alami, M. Schön, M. Orth, S. Liebau, G. Barbi, A. M. Grabrucker, R. Delorme, M. Fauler, B. Mayer, S. Jesse, F. Roselli, A. C. Ludolph, T. Bourgeron, C. Verpelli, M. Demestre, T. M. Boeckers, Autism-associated SHANK3 mutations impair maturation of neuromuscular junctions and striated muscles. Sci. Transl. Med. 12, eaaz3267 (2020).
Figure: Skeletal muscle biopsies of patients with PMDS at different ages and age-matched controls were analysed. (B) Sagital human skeletal muscle from a healthy donor were labelled with SHANK3 (green)/alpha-ACTININ (red) demonstrating strong SHANK3 localisation at the muscle sarcomere. (Picture extracted from Lutz et al., Science Translational Medicine 2020).





